Anatomic overview:






Thyroid nodules are common and occur in up to 50% of the adult population; however, less than 7% of thyroid nodules are malignant. Microcalcifications are one of the most specific US findings of a thyroid malignancy.
Other useful US features include a marked hypoechogenicity, irregular margins, and the absence of a hypoechoic halo around the nodule.
Lymphadenopathy and local invasion of adjacent structures are highly specific features of thyroid malignancy but are less commonly seen.
The number, size, and interval growth of nodules are nonspecific characteristics. A functioning, or “hot,” thyroid nodule is rarely malignant, with only a few reported cases of such malignancy. Although a nonfunctioning, or “cold,” nodule at scintigraphy is commonly thought to indicate an increased risk of thyroid malignancy, as many as 77% of cold thyroid nodules may be benign. The main pathologic types of thyroid carcinoma are papillary, follicular, medullary, and anaplastic. Metastases to the thyroid are rare and usually originate from primary lung, breast, and renal cell carcinomas. Metastatic disease should be suspected when a solid thyroid nodule is found in a patient with a known nonthyroid malignancy.
Thyroid calcifications may occur in both benign and malignant disease. Thyroid calcifications can be classified as microcalcification, coarse calcification, or peripheral calcification. At US, microcalcifications appear as punctate hyperechoic foci without acoustic shadowing. Large irregularly shaped dystrophic calcifications also may occur and are secondary to tissue necrosis. They are commonly present in multinodular goiters; however, when found in solitary nodules, they may be associated with a malignancy rate of nearly 75%. Coarse calcifications may coexist with microcalcifications in papillary cancers, and they are the most common type of calcification in medullary thyroid carcinomas.
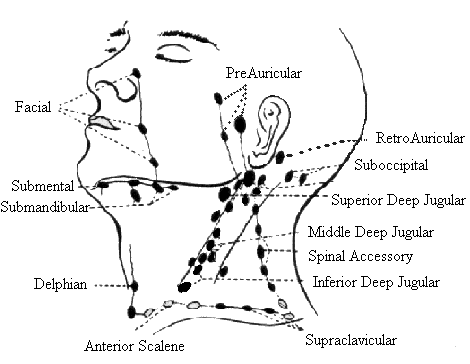
Metastases to regional cervical lymph nodes have been reported to occur in 19.4% of all thyroid malignancies. They are most common in papillary thyroid carcinoma. US features that should arouse suspicion about lymph node metastases include a rounded bulging shape, increased size, replaced fatty hilum, irregular margins, heterogeneous echotexture, calcifications, cystic areas , and vascularity throughout the lymph node instead of normal central hilar vessels at Doppler imaging.
The halo or hypoechoic rim around a thyroid nodule is produced by a pseudocapsule of fibrous connective tissue, a compressed thyroid parenchyma, and chronic inflammatory infiltrates. A completely uniform halo around a nodule is highly suggestive of benignity. Nodules can be classified according to their contours as smooth and rounded or irregular with jagged edges. An ill-defined and irregular margin in a thyroid tumor suggests malignant infiltration of adjacent thyroid parenchyma with no pseudocapsule formation. The most common pattern of vascularity in thyroid malignancy is marked intrinsic hypervascularity, which is defined as flow in the central part of the tumor that is greater than that in the surrounding thyroid parenchyma.
A completely avascular nodule is very unlikely to be malignant.
SUMMARY:
Malignant nodules, both carcinoma and lymphoma, typically appear solid and hypoechoic when compared with normal thyroid parenchyma. The size of a nodule is not helpful for predicting or excluding malignancy. However, in general, smaller malignancies have a more favorable prognosis than do larger lesions. In general, interval growth of a thyroid nodule is a poor indicator of malignancy. Benign thyroid nodules may change in size and appearance over time, with the potential to either enlarge or decrease in size. Abnormal lymph nodes adjacent to the thyroid gland may be mistaken for benign nodules in a multinodular thyroid, especially if the nodes are cystic or calcified. US characteristics of autoimmune diseases such as Graves disease or chronic lymphocytic (Hashimoto) thyroiditis include enlargement of the thyroid with reduced echogenicity, heterogeneity, and hypervascularity, particularly in Graves disease. Diffusely infiltrative papillary or follicular thyroid carcinoma may have all these features and therefore may be mistaken for autoimmune thyroid disease. US features that are suggestive of malignancy include irregular or nodular enlargement of the thyroid gland, sparing from the infiltrative process in parts of the gland, and nodal metastases.
Palpable thyroid nodules should be investigated with FNA on the basis of thyroid function test results, clinical presentation, US features, and risk factors. Consensus guidelines set by the Society of Radiologists in Ultrasound are based on the size of the nodule and suspicious US characteristics. FNA is recommended for the following: microcalcifications in a nodule with a diameter of 1 cm or greater; coarse calcification or a solid nodule with a size of 1.5 cm or greater; and a mixed cystic and solid nodule with a size of 2 cm or greater. US is valuable for identifying many malignant or potentially malignant thyroid nodules. Although there is some overlap between the US appearance of benign nodules and that of malignant nodules, certain US features are helpful in differentiating between the two. These features include microcalcifications, local invasion, lymph node metastases, a nodule that is taller than it is wide, and markedly reduced echogenicity. Other features, such as the absence of a halo, ill-defined irregular margins, solid composition, and vascularity, are less specific but may be useful ancillary signs. Apart from local extrathyroidal invasion, none of these features is individually pathognomonic of malignancy. However, in combination, these features may lead to a diagnosis of malignancy and may direct attention to other suspicious nodules in need of further investigation. Potential diagnostic pitfalls include routinely dismissing small nodules, assuming that multiple nodules are most likely benign, mistaking carcinomas for cystic hyperplastic nodules and Graves disease, and mistaking adjacent nodal metastases for benign thyroid nodules.
----------------------------------------------------------------------------------------------------------------------------------------
FNA:
Indications:
Presence of a solitary nodule, >10mm in case of microcalcifications, >15mm in case of solid nodules or in the presence of coarse calcifications.
Whenever clinical information or US features arouse suspicion of malignancy.
Rapid growth.
Multiple nodules have the same risk of malignancy as a single nodule. In case of an autoimmune inflammatory process the rate of malignancy is simillar to a non-symptomatic gland.
Signs of malignant leasion:
Microcalcifications
Marked hypoechogenicity
Irregular microlobulated margin
Longitudinal dimension larger than crossectional dimension
Intrinsic vascularity
Invasion af adjacent tissue
Mets to l.n.
Risk factors for malignancy:
+ family history
Irradiation to the neck region
Male
<30, >60 years old
Type II multiple endocrine neoplasia
----------------------------------------------------------------------------------------------------------------------------------------
3.1 cm thyroid nodule containing colloid
Link: http://www.ultrasound-images.com/thyroid.htm#Follicular_adenoma
----------------------------------------------------------------------------------------------------
centralisan többszörösen septált cystosus részt tartalmazó göb van.
LINKS:
(Text source: Radiographics magazine - US Features of Thyroid Malignancy pearls and pitfalls may 2007 )
(Images: Pecs Universitey Department of Radiology, Ultrasoundcases.info )
I was having chronic problems with mid afternoon exhaustion and then wide awake at night. I had tried everything to boost my energy level and nothing worked. I started taking herbal thyroid supplements and within a week i felt like a normal person again
ReplyDelete